|
Consideration of emerging evidence relevant to pediatrics has prompted the American Diabetes Association (ADA) to revise its hemoglobin A 1c (A1C) targets in pediatric T1D several times through the years. These advances have also contributed to lessening hypoglycemia risk and have diminished the relationship of significant or severe hypoglycemia with lower glycemic targets in people with T1D. The development of insulin analogs, more sophisticated insulin delivery systems (e.g., insulin pumps), continuous glucose monitoring (CGM), and, more recently, integrated systems (e.g., sensor-augmented insulin pumps, predictive low-glucose suspend systems, and closed-loop control systems) greatly enhanced the feasibility of maintaining glucose levels within a prespecified target range. Since its 1993 landmark publication, the DCCT and many other studies have progressively provided overwhelming evidence that near-normal glucose control diminishes the risks of retinopathy, nephropathy, neuropathy, and macrovascular complications ( 4). 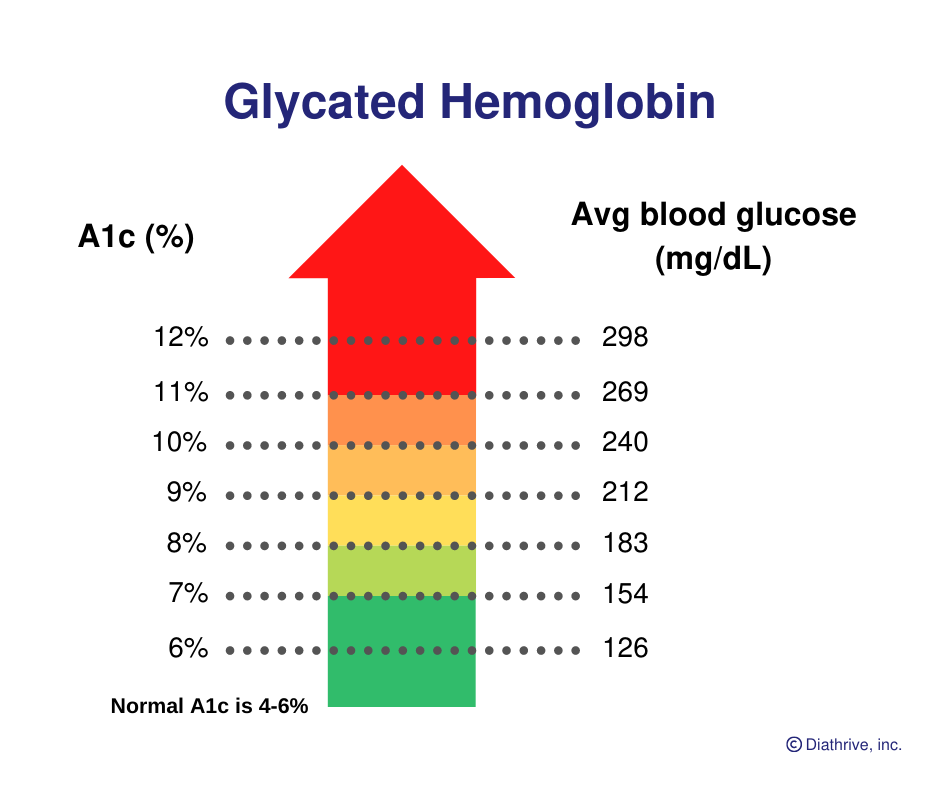
We aim to raise awareness within the community on Standards of Care updates that impact this crucial goal in pediatric diabetes management. We present common barriers to achieving glycemic targets in pediatric diabetes and discuss some strategies to address them. We also review data supporting a decrease over time in overall severe hypoglycemia risk for youth with T1D, partly associated with the use of newer insulins and devices, and weakened association between lower A1C and severe hypoglycemia risk. Here, we provide a historical perspective of A1C targets in pediatrics and highlight evidence demonstrating detrimental effects of hyperglycemia in children and adolescents, including increased likelihood of brain structure and neurocognitive abnormalities, microvascular and macrovascular complications, long-term effects, and increased mortality. During the “honeymoon” period and in situations where lower mean glycemia is achievable without excessive hypoglycemia or reduced quality of life, an A1C <6.5% may be safe and effective. Even less stringent A1C targets (e.g., <8%) may be warranted for children with a history of severe hypoglycemia, severe morbidities, or short life expectancy. A higher A1C target of <7.5% may be more suitable for youth who cannot articulate symptoms of hypoglycemia or have hypoglycemia unawareness and for those who do not have access to analog insulins or advanced diabetes technologies or who cannot monitor blood glucose regularly. We are not a laboratory and are unable to comment on an individual's health and treatment.The American Diabetes Association 2020 Standards of Medical Care in Diabetes (Standards of Care) recommends a hemoglobin A 1c (A1C) of <7% (53 mmol/mol) for many children with type 1 diabetes (T1D), with an emphasis on target personalization. Lab Tests Online-UK is an educational website designed to provide patients and carers with information on laboratory tests used in medical care. 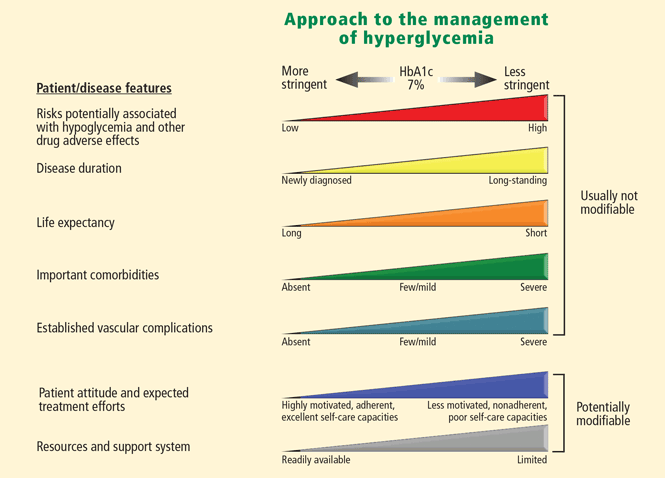
If you are concerned about your test results, you will need to arrange an appointment with your doctor so that all relevant information including age, ethnicity, health history, signs and symptoms, laboratory and other procedures (radiology, endoscopy, etc.), can be considered. If the doctor wants to see you about the result(s), you will be offered an appointment. Your GP practice will be able to provide specific details. If you are registered to use the online services of your local practice, you may be able to access your results online. The X-ray & scan results may take longer. Some specialist test results may take longer, if samples have to be sent to a reference (specialist) laboratory. On average it takes 7 working days for the blood test results to come back from the hospital, depending on the exact tests requested.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
